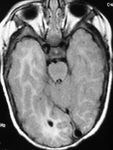
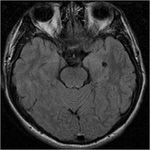
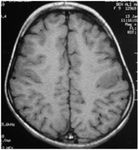
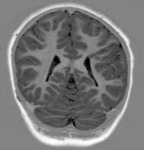
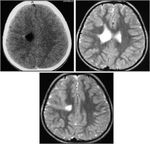
I. Major phases of cerebral cortical development:
The human cortex develops its basic structure during the first two trimesters of pregnancy as a series of overlapping steps:
-Between the second and fourth months of gestation.
-Anomalies of neuronal proliferation may result in conditions characterized by too many, too few, or abnormal neurons.
-Between the third and fifth months of gestation.
-Disorders of neuronal migration are due to undermigration, overmigration, or ectopic migration of the neurons.
- Postmigrational cortical development:
-Starts at 22 weeks of fetal gestation and continues until 2 years of age.
-Disorders of cortical organization result in abnormalities of gyral formation and cortical organization.
II. Classification:
The revised Barkovich classification is most widely accepted, and is based on the proposed underlying mechanisms with a mixture of genetic and imaging criteria.
The classification system is broadly based on the following categories:
1. Abnormal cell proliferation or apoptosis
1.1 Abnormal brain size
a.Microcephaly
b.Macrocephalies (megalencephaly/macrocephaly)
1.2 Abnormal cell proliferation
a.Non-neoplastic
-Cortical hamartomas of tuberous sclerosis
-Hemimegalencephaly
-Focal cortical dysplasia (Type I and Type IIb)
b.Neoplastic
-Ganglioglioma
-Gangliocytoma
-Dysembryoplastic neuroepithelial tumor (DNET)
2.Abnormal neuronal migration
2.1.Lissencephaly
2.2.Heterotopia: ectopic migration
3.Abnormal cortical organization
3.1.Mild malformations of cortical development (previously microdysgenesis)
3.2 Polymicrogyria and schizencephaly
a.Bilateral polymicrogyria syndromes
b.Schizencephaly
3.3.Focal cortical dysplasia (Type IIa)
4. Not otherwise classified
4.1 Malformations secondary to inborn errors of metabolism
4.2. Other unclassified malformations
The malformations microcephaly, cortical dysplasia, hemimegalencephaly, lissencephaly, heterotopia, polymicrogyria and schizencephaly will be presented with their clinical and imaging features.
Disorders of proliferation:
1- Microcephaly with simplified gyration (MSG):
a.MRI features of MSG
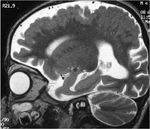
Fewer glia and/or neurons result in a small brain (microcephaly). This is generally associated with a more or less simplified gyral pattern. Gyration is less complex and the number of gyri is reduced. There is a continuum between normal gyration and a simplified pattern however, and a clear distinction is not always possible.
b.Clinical features of MSG
In children with autosomal recessive microcephaly with simplified gyral pattern, head circumference is more than 3 SD below the mean. Children are generally mentally retarded, but show no specific neurological abnormalities such as epilepsy or spasticity.
2- Hemimegalencephaly:
Hemimegalencephaly or unilateral megalencephaly is a rare but well-known congenital malformation characterized by enlargement of all or parts of a cerebral hemisphere. The affected hemisphere may have focal or diffuse neuronal migration defects, with areas of polymicrogyria pachygyria, and heterotopia.
a.MRI features of MSG:
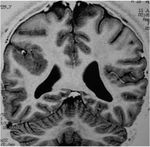
In addition to excessive growth limited to 1 cerebral hemisphere, MR imaging studies have revealed various other abnormalities accompanying this condition, such as enlargement of the lateral ventricle, an abnormal gyral pattern with a thick cortex, gliosis in the white matter on the affected side, and abnormal myelination.
b.Clinical features of MSG:
Symptoms of megalencephaly may include delayed development, convulsive disorders, corticospinal (brain cortex and spinal cord) dysfunction, and seizures.
3-Cortical dysplasia:
a.Clinical features of cortical dysplasia:
Cortical dysplasias are highly epileptogenic, and are rigorously sought for in children with intractable focal epilepsy, as they are the most frequent cause of focal refractory seizures in this age group.
b.MRI features of cortical dysplasia:
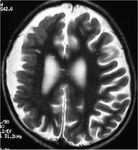
Clues to look for are focal cortical thickening, blurred gray-white matter junction and related 'migration lines'. These are gray matter lines in the subcortical white matter. If these are visible and extend to the lateral ventricle, the abnormality is called a transmantle dysplasia. MRI features suggestive of a type II cortical dysplasia are increased cortical thickness, transmantle signs and FLAIR or T2 weighted signal change. Migration lines and the gray-white matter junction are best appreciated on T1 weighted imaging. T2 weighted images or FLAIR images show associated white matter hyperintensity or gliosis.
Disorders of migration:
1- Lissencephaly:
a. MRI features:
In the lissencephaly-pachygyria-subcortical band heterotopia spectrum, MRI features can distinguish well between the different types of lissencephaly. In type 1 or classic lissencephaly the cortex is smooth and thickened (>10mm) with a cell sparse zone. Milder types of lissencephaly show thickened gyri (pachygyria) or fairly normal gyri with a band of gray matter below, the subcortical band heterotopia, consisting of neurons arrested during migration.
b. Clinical feature of lissencephaly:
Lissencephaly type I was the earliest recognized MCD, and consequently much is known about the clinical features. Signs and symptoms are very diverse and range from normal intelligence to severe mental retardation. There is a relationship between the severity of the lissencephaly/pachygyria grading based on neuroimaging and outcome with respect to the severity of psychomotor retardation, motor symptoms and epilepsy. Most to all patients have epilepsy.
2- Heterotopia:
a. MRI features of heterotopia:
Heterotopia are formed of neurons that have not migrated to their destination in the cortex. As they are otherwise normal neurons, they have all characteristics of gray matter on MRI. Heterotopia can be unilateral or bilateral, and isolated versus continuous. Bilateral continuous periventricular heterotopia with an otherwise normal brain, except for an enlarged retrocerebellar space, is the classical phenotype of FLNA mutations.
b. Clinical features of heterotopia:
Clinical features are very diverse. Psychomotor development may be completely normal or delayed. Periventricular nodular heterotopias give a high risk of epilepsy, but seizures may be delayed until adulthood.
Disorder of cortical organization:
1- Polymicrogyria:
Polymicrogyria is the most heterogeneous malformation of cortical development, both in appearance as in causes. It can be seen as an isolated malformation, but also in combination with periventricular nodular heterotopia or other brain malformations such as corpus callosum agenesis or cerebellar abnormalities.
a. MRI features of polymicrogyria:
Polymicrogyria is probably the most common MCD. In newborns the cortex is thin and due to a lack of myelination the gray-white matter border is harder to appreciate. In these infants the polymicrogyric cortex shows numerous, very small ripples. After myelination the polymicrogyric cortex appears thickened with an unclear white-matter junction. The surface of the cortex may appear lumpy-bumpy or may seem smooth due to fusion of the upper layer of the cortex across adjacent microgyri.
b. Clinical features of polymicrogyria:
Bilateral perisylvian polymicrogyria results in the so-called perisylvian syndrome. Motor function of the oral musculature is impaired, resulting in speech delay, dysarthria and dysphagia.
2- Schizencephaly:
a. MRI features of schizencephaly:
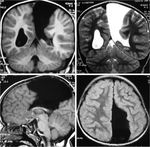
Schizencephaly appears as a cleft filled with CSF and extending medially from the subarachnoid space into the lateral ventricle. The wall of the cleft is lined with dysmorphic gray matter. The gray matter sometimes extends into the lateral ventricle in the form of subependymal heterotopias. The cleft may be small or large, unilateral or bilateral. The anomaly may be of the open-lip or closed-lip type. Closed-lip schizencephaly is characterized by gray matter–lined lips, which are in contact with each other (type 1). Open-lip schizencephaly has separated lips and a cleft of CSF extending to the underlying ventricles (type 2)
b. Clinical features of schizencephaly:
Clinical manifestations of schizencephaly most often include varying degrees of developmental delay, motor impairment, and seizures. It might be associated with septo-optic dysplasia, optic nerve hypoplasia or the absence of septum pellucidum, pachygyria, PMG, heterotopia, and arachnoid cysts.